Joint mobilisation is a hands-on treatment that physiotherapists use to reduce pain, restore movement, and improve how a joint functions. But not all mobilisation is the same. The technique is graded from a very gentle, almost imperceptible movement to a firm, end-range push and that grading system matters enormously.
The framework most widely used today was developed by physiotherapist Geoffrey Maitland in the 1960s and has since been refined through decades of clinical research. It gives clinicians a shared language and a systematic way to match treatment intensity to what the patient actually needs. Understanding these grades can help you feel less anxious about treatment, ask better questions, and understand why your physiotherapist might change their approach from session to session.
This article explains each of the five grades of mobilisation clearly, describes what each one feels like, and outlines when they are – and are not appropriate to use.
What Is Joint Mobilisation?
Joint mobilisation is a manual therapy technique. The physiotherapist applies a controlled, passive movement to a joint – meaning you are not actively moving it yourself; they are moving it for you. The movement can be applied to the spine (neck, mid-back, lower back) or to peripheral joints such as the shoulder, hip, knee, or ankle.
The goal can vary depending on the grade used:
- Reduce pain (especially acute or irritable pain)
- Improve range of movement (when a joint feels stiff or restricted)
- Restore normal joint mechanics (when a joint is not moving the way it should)
- Stimulate mechanoreceptors (nerve endings in the joint that influence pain processing)
Mobilisation is different from manipulation. Manipulation (Grade V, sometimes called a High-Velocity Low-Amplitude thrust) is a faster, more forceful technique. Grades I-IV are mobilisations – slower, smoother, more controlled. Both have their place, but they are not interchangeable.
The Maitland Grading System Explained
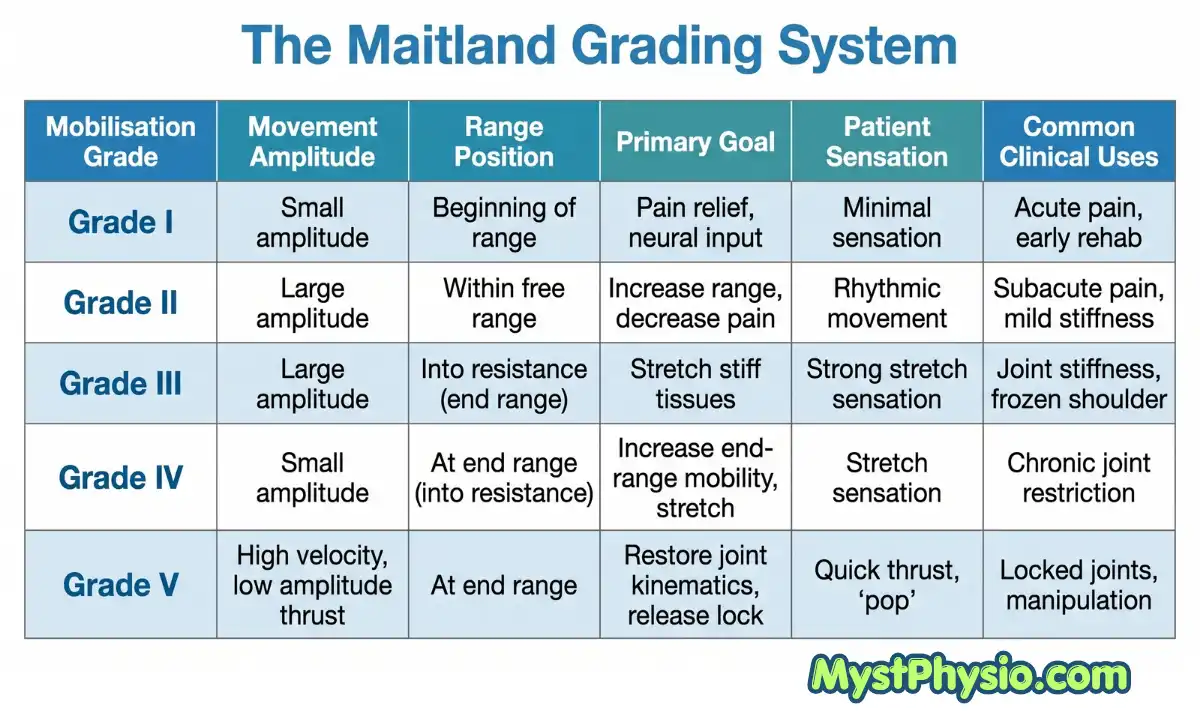
The Maitland Concept divides joint mobilisation into five grades based on two key factors: the amplitude of the movement (how large the oscillation is) and where in the joint’s available range the movement occurs.
To understand this, picture a joint’s range of motion as a line – from the starting position at one end to the absolute limit of movement (the “end of range”) at the other. The joint becomes progressively stiffer as you move toward that end. Maitland called this resistance point R1, and the absolute end-of-range limit R2.
Grade I Mobilisation
Grade I involves small-amplitude oscillations (rhythmic back-and-forth movements) performed at the very beginning of the joint’s available range. There is no movement into resistance whatsoever.
This grade is chosen primarily for pain relief, particularly when a joint is very irritable – meaning even small amounts of movement cause significant pain. In this situation, a gentle Grade I technique can stimulate mechanoreceptors in the joint capsule, which helps modulate (dampen) pain signals travelling to the brain. This is sometimes explained through the “gate control theory” of pain.
From a patient’s perspective, it barely feels like anything is happening. That is intentional.
Typical uses: Acute spinal pain, highly irritable shoulder conditions, post-surgical early-stage rehabilitation.
Grade II Mobilisation
Grade II still involves larger-amplitude oscillations, but they remain within the range before resistance begins. The movement is smooth and rhythmic, passing through the free (non-restricted) part of the joint’s range without ever reaching stiffness or end-of-range.
Like Grade I, it is primarily used for pain modulation. However, because the amplitude is larger, it can also begin to address mild movement restriction in relatively pain-free joints.
In my clinical work, I reach for Grade II mobilisations frequently in the early stages of treatment – particularly when a patient is guarding heavily or has a high pain state. Building trust with the joint before progressing is nearly always the right approach.
Typical uses: Subacute neck pain, early shoulder impingement, mild joint stiffness with significant pain sensitivity.
Grade III Mobilisation
Grade III is where things shift. The oscillations are large in amplitude but now move into the resistance at the end of the available range. The physiotherapist pushes into where the joint begins to stiffen and oscillates rhythmically within that resistant zone.
This grade is primarily aimed at improving range of movement. It stretches the joint capsule, surrounding ligaments, and other periarticular (around the joint) structures. It tends to feel more noticeable and may reproduce some discomfort, but should not cause sharp or worsening pain.
A clinician will always monitor your response carefully during and after a Grade III technique. If pain significantly increases, it is an indication to step back.
Typical uses: Chronic stiff shoulder (adhesive capsulitis, sometimes called “frozen shoulder”), restricted cervical spine in subacute stage, limited ankle dorsiflexion (the movement that brings your toes upward).
Grade IV Mobilisation
Grade IV consists of small-amplitude oscillations performed at the very end of the available range – firmly into resistance. The physiotherapist is working right at the limit of what the joint currently allows.
This is the most targeted of the mobilisation grades. It stretches very specific, localised areas of capsular tightness or fibrosis (scar-like thickening of soft tissue). The force applied is greater than in Grade III, and it may provoke local discomfort, particularly if the joint has significant restriction.
Patients often describe it as a “stretching feeling” or “a bit uncomfortable but bearable.” That response is expected. If it produces sharp, shooting, or radiating pain, it should stop.
Typical uses: Chronic stiff joints, long-standing restricted lumbar or cervical facet joints, glenohumeral (shoulder ball-and-socket) capsular tightness.
Grade V Mobilisation (Manipulation)
Grade V is technically classified within the Maitland framework, though it is qualitatively different from Grades I-IV. It is a High-Velocity Low-Amplitude (HVLA) thrust – a very quick, precise movement applied at the end of range.
This is what produces the “cracking” sound that many people associate with spinal manipulation. That sound is called a cavitation – it is caused by a rapid change in pressure within the joint fluid, not by bones cracking or breaking.
Grade V is not appropriate for every patient or every joint. It requires thorough screening to rule out contraindications (reasons why it would be unsafe) such as:
- Osteoporosis (weakening of bone density)
- Inflammatory arthritis in an active flare
- Ligamentous instability
- Vascular abnormalities (particularly relevant for cervical spine manipulation)
- Previous joint surgery in the area
When appropriate, it can be very effective for certain types of acute locked back or neck presentations. It must only be performed by a trained and registered physiotherapist or chiropractor who has completed the required post-graduate competency.
RELATED: 7 Best Physiotherapy Exercises for Bell’s Palsy Recovery
How Does a Physiotherapist Choose the Right Grade?
This is where clinical reasoning – not just textbook knowledge – comes in. The choice of grade depends on several factors assessed at each appointment:
- Pain level and irritability of the joint – how easily pain is provoked and how long it takes to settle
- The stage of the condition – acute (new), subacute (settling), or chronic (long-standing)
- What the joint assessment reveals – is movement restricted by pain alone, or by stiffness, or both?
- The patient’s tolerance and response – feedback during treatment drives real-time adjustment
A common clinical principle is: use lower grades (I-II) when pain dominates, and progress toward higher grades (III-IV) when stiffness dominates. It is rarely one or the other, and an experienced physiotherapist will often blend techniques within a single session.
Response to treatment should always be reassessed. If a Grade III mobilisation leaves the joint more painful the following day, it is not an automatic sign to stop – but it is essential information that shapes the next session.
Contraindications and Precautions
Joint mobilisation is generally safe, but it is not appropriate in every situation. Physiotherapists are trained to identify red flags (signs of serious underlying pathology) before any hands-on treatment begins.
Absolute contraindications (where mobilisation should not be used):
- Malignancy (cancer) involving the bone or joint area
- Active infection in or around the joint
- Acute fracture
- Severe rheumatoid arthritis instability (particularly at the upper cervical spine)
- Uncontrolled neurological signs (e.g., progressive weakness or loss of bladder/bowel control)
Relative precautions (where mobilisation may be used, but with caution and modification):
- Osteoporosis
- Pregnancy (particularly lumbar mobilisation in later trimesters)
- Anticoagulant therapy (blood-thinning medication)
- Hypermobility syndromes (e.g., Ehlers-Danlos Syndrome, where joints are already too loose)
If you have any of these conditions, always disclose them at your first appointment. It will not necessarily prevent treatment, but it will change how your physiotherapist approaches it.
What the Evidence Says
The use of joint mobilisation is supported by a substantial body of research, though the evidence varies by grade and condition.
A 2022 systematic review published in the Journal of Manual and Manipulative Therapy confirmed that Grades III and IV spinal mobilisation produce clinically meaningful short-term reductions in pain and disability in people with chronic low back pain. A 2020 Cochrane review found moderate-quality evidence supporting manual therapy (including joint mobilisation) for shoulder pain, particularly in the short term. For cervicogenic headache (headaches originating from neck dysfunction), mobilisation of the upper cervical spine has demonstrated significant effectiveness compared to no treatment in multiple randomised controlled trials.
It is important to note that mobilisation is rarely used in isolation. It is most effective when combined with targeted exercise rehabilitation, patient education, and where appropriate, lifestyle modification.
Frequently Asked Questions (FAQs)
It depends on the grade used and the state of your joint. Grades I and II should cause little to no discomfort. Grades III and IV may reproduce some local aching or stretching sensation, which is expected and usually settles quickly after treatment. You should never feel sharp, shooting, or worsening neurological symptoms (numbness, tingling, spreading pain) during mobilisation – if you do, tell your physiotherapist immediately.
This varies considerably. Some people notice a meaningful change in pain or movement after one or two sessions. Others with chronic, long-standing stiffness may need four to six sessions before significant improvement accumulates. Your physiotherapist should reassess and explain progress clearly at each visit.
In many cases, yes. Osteoarthritis (the age-related “wear and tear” type) is not a contraindication to mobilisation – in fact, graded mobilisation is a recommended component of conservative arthritis management. Active inflammatory arthritis (such as rheumatoid arthritis in a flare) is a different matter and requires careful assessment.
Yes. Mobilisation (Grades I-IV) is slow, controlled, and rhythmic – the patient can stop it at any time. Manipulation (Grade V) is a single, rapid thrust technique. Both are forms of manual therapy, but they have different indications, risks, and skill requirements. Not all physiotherapists perform Grade V manipulation; additional post-graduate training is required.
Some mild local soreness for 12-24 hours is common and is not a cause for alarm. Applying a heat pack to the area can help. Your physiotherapist may give you specific exercises to do at home between sessions – these are important for maintaining and building on the gains made during treatment. Avoid heavy loading or high-intensity activity of the treated joint on the day of treatment unless instructed otherwise.
Conclusion
The five grades of joint mobilisation – from the barely perceptible Grade I through to the end-range precision of Grade IV and the thrust of Grade V – are not arbitrary labels. They represent a calibrated, evidence-informed system that allows a skilled physiotherapist to match the intensity and type of movement to exactly what your joint needs at that moment in your recovery.
Understanding these grades helps you be an active participant in your own rehabilitation – not just a passive recipient of treatment. If something feels wrong during a session, say so. If you’re not seeing change after several sessions, ask why. That dialogue between patient and clinician is part of how good physiotherapy works.
Consult your doctor or a qualified physiotherapist for a personalised assessment before starting any manual therapy treatment.
References
- Coulter ID, Crawford C, Hurwitz EL, et al. Manipulation and mobilization for treating chronic low back pain: a systematic review and meta-analysis. Spine Journal. 2022;18(5):866-879. https://doi.org/10.1016/j.spinee.2018.01.013
- Page MJ, Green S, McBain B, et al. Manual therapy and exercise for rotator cuff disease. Cochrane Database of Systematic Reviews. 2020;(6):CD012224.
- Jull G, Trott P, Potter H, et al. A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine. 2022;27(17):1835-1843. https://doi.org/10.1097/00007632-200209010-00004
- Maitland GD, Hengeveld E, Banks K, English K. Maitland’s Vertebral Manipulation (8th ed.). Edinburgh: Elsevier Butterworth-Heinemann; 2013.
- Vicenzino B, Paungmali A, Teys P. Mulligan’s mobilization-with-movement, positional faults and pain relief: current concepts from a critical review of literature. Manual Therapy. 2022;12(2):98-108. https://doi.org/10.1016/j.math.2006.07.012
- National Institute for Health and Care Excellence (NICE). Low back pain and sciatica in over 16s: assessment and management (NICE Guideline NG59). London: NICE; 2022. https://www.nice.org.uk/guidance/ng59
- Mintken PE, DeRosa C, Little T, Smith B. A model for standardizing manipulation terminology in physical therapy practice. Journal of Manual and Manipulative Therapy. 2020;16(1):50-56. https://doi.org/10.1179/106698108790818567



