You rested it. You iced it. You backed off training for two weeks. And then it came back.
That slow, nagging ache in your heel, elbow, or shoulder that just won’t fully go away? There’s a name for it: tendinopathy. And the reason it keeps returning has everything to do with how tendons actually heal, which is very different from how most people think.
What Is Tendinopathy?
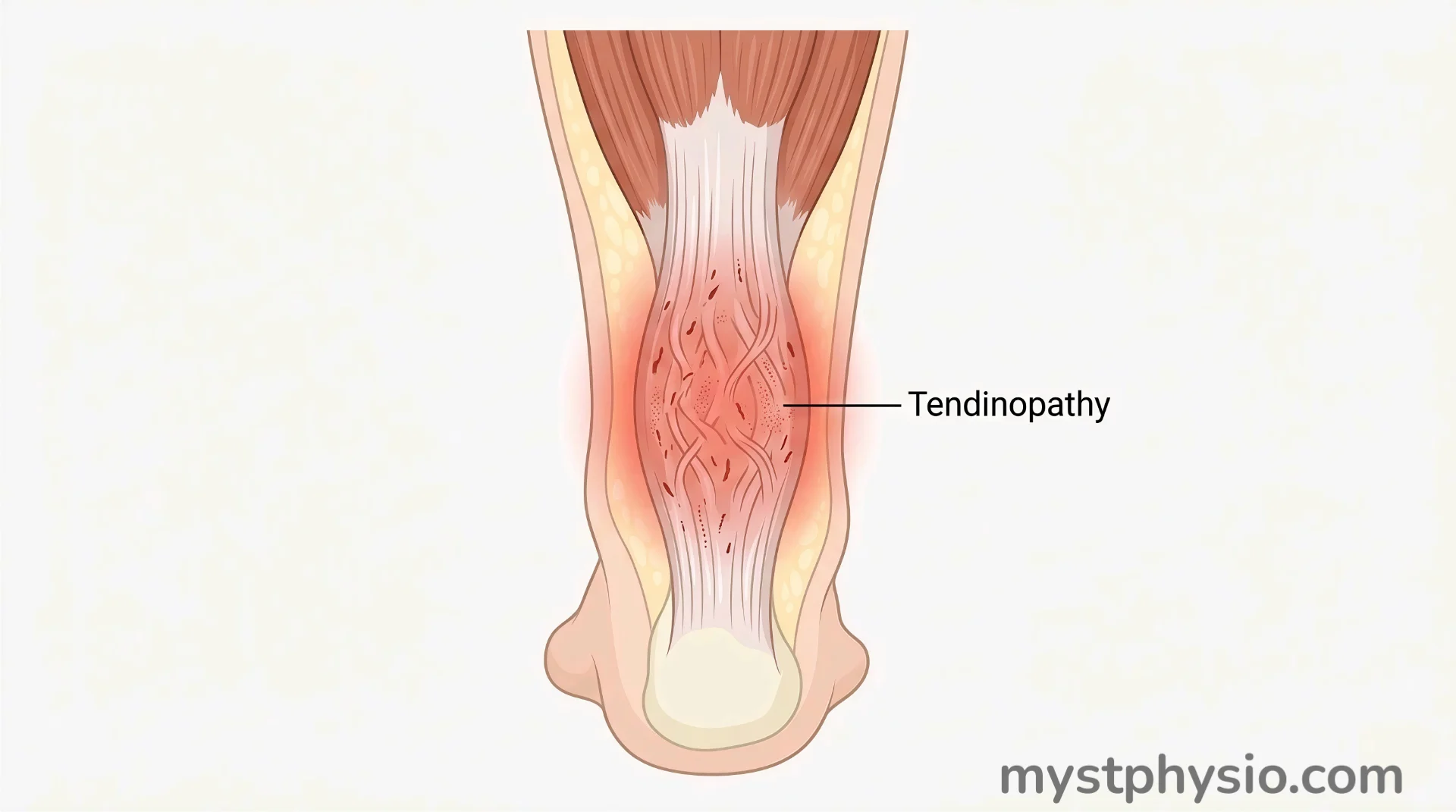
A tendon is a thick, rope-like cord of tissue. It connects your muscle to your bone. Every time you move, jump, grip, or run, your tendons take the force.
Tendinopathy (ten-din-OP-uh-thee) is an umbrella term. It simply means the tendon is damaged and not working properly. It covers everything from early irritation to long-term degeneration (breakdown of the tendon’s internal structure).
You might also hear older terms like tendinitis (meaning inflammation) or tendinosis (meaning tissue breakdown without inflammation). Most specialists now prefer “tendinopathy” because it covers the full picture.
Where Does It Happen?
Tendinopathy can strike almost any tendon, but some are more vulnerable than others:
- Achilles tendon – back of the ankle; very common in runners
- Patellar tendon – below the kneecap; often affects jumpers and cyclists
- Rotator cuff tendons – in the shoulder; common in people who work overhead
- Common extensor tendon – outer elbow; the classic “tennis elbow”
- Gluteal tendons – outer hip; frequently affects middle-aged women
Why Does Tendon Pain Keep Coming Back?
This is the part that trips most people up. And honestly, it tripped up the medical world for years too.
Tendons Heal Slowly – Much More Slowly Than Muscle
Muscle has a rich blood supply. When muscle gets injured, nutrients and repair cells rush in fast. Tendons, by contrast, have very poor blood flow. Especially in the middle portion of the tendon, where most damage actually occurs.
That means healing is slow. Not days. Not weeks. Months, sometimes longer.
When you “rest and feel better,” your pain often disappears before the tendon has actually repaired itself. You feel fine, you load it again, and the pain is back. This cycle is one of the most frustrating things about tendinopathy.
The Tendon Changes at a Cellular Level
Inside a healthy tendon, fibres line up in neat, parallel rows. They’re organised. Strong. Efficient.
In a damaged tendon, those fibres get disorganised. New, weaker fibres grow in random directions. The tendon becomes thickened, less springy, and more vulnerable to load. Research published in journals including the British Journal of Sports Medicine confirms that this structural change, called tendon disrepair, can persist even when your pain has gone.
This is why pain is a terrible guide to tendon health. The tendon can feel fine and still be structurally compromised.
You Can’t Fully Rest Your Way to Recovery
Here’s something counterintuitive: complete rest actually makes tendons weaker over time.
Tendons need mechanical load. They need to be stressed in a controlled way to stimulate repair. Without any load, the disorganised fibres never reorganise. The tendon becomes stiff and less able to handle normal activity. When you return to sport or work, it flares again.
The goal isn’t rest. It’s the right kind of loading.
RELATED: What Happens Inside a Frozen Shoulder? Adhesive Capsulitis Explained Clinically
What Actually Helps Tendinopathy Heal
Heavy Slow Resistance Training
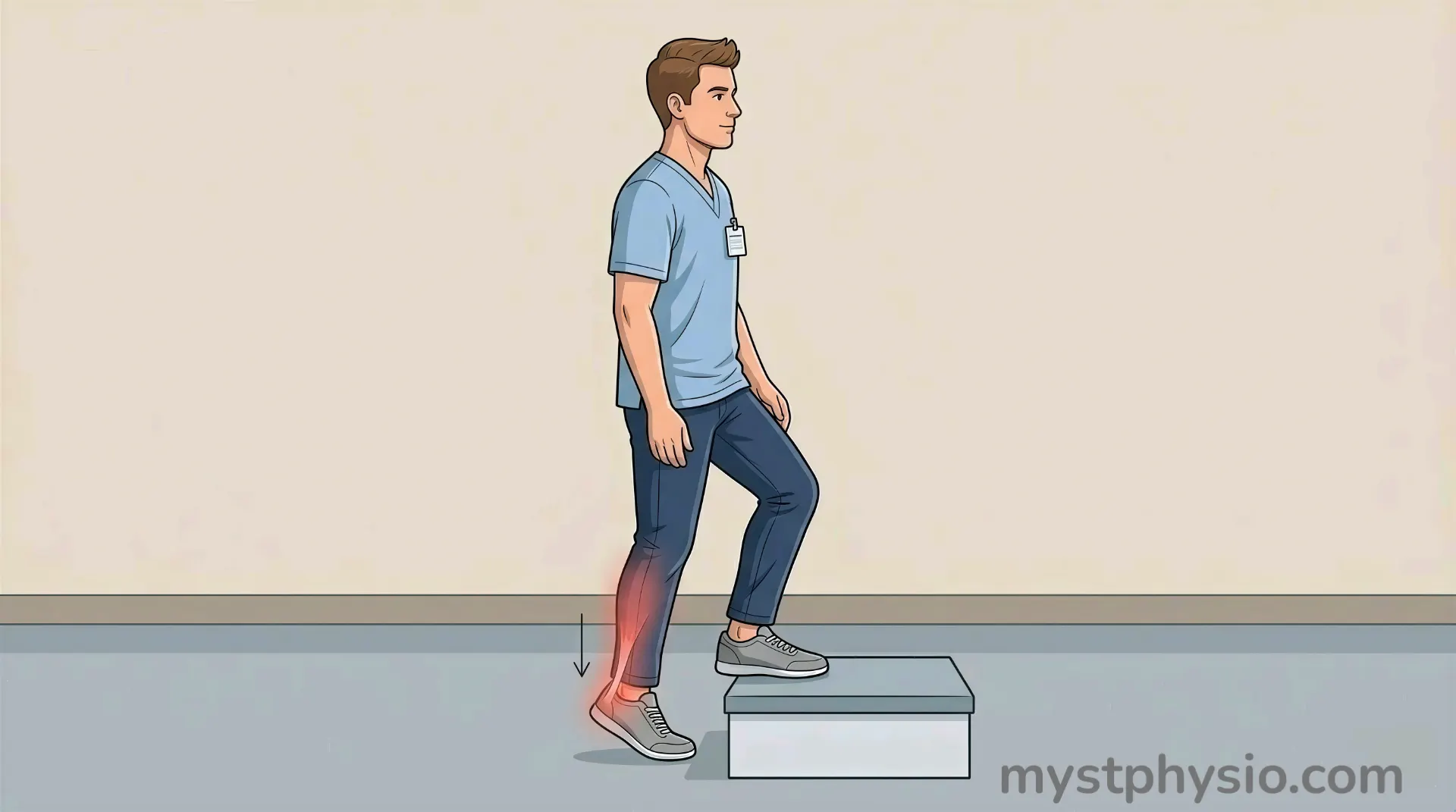
This is the most evidence-backed approach for most tendinopathies. The research is consistent and robust.
Heavy slow resistance (HSR) training means loading the tendon with significant weight, performed slowly and with control. Think slow, deliberate heel raises for Achilles tendinopathy. Or slow, weighted knee extensions for patellar tendinopathy.
The “slow” part matters. It keeps the load on the tendon longer, stimulating more repair without jerky forces that cause further damage.
A typical programme involves:
- 3-4 sets of 6-8 repetitions
- 3-second up, 3-second hold, 3-second down (sometimes written as 3-0-3 tempo)
- 3-4 sessions per week
- Progressive increase in load over 8-12 weeks
This is not something to jump into alone. A physiotherapist (sometimes called a physical therapist) should guide your programme, especially in the early stages.
Isometric Exercises – The Pain Relief Trick
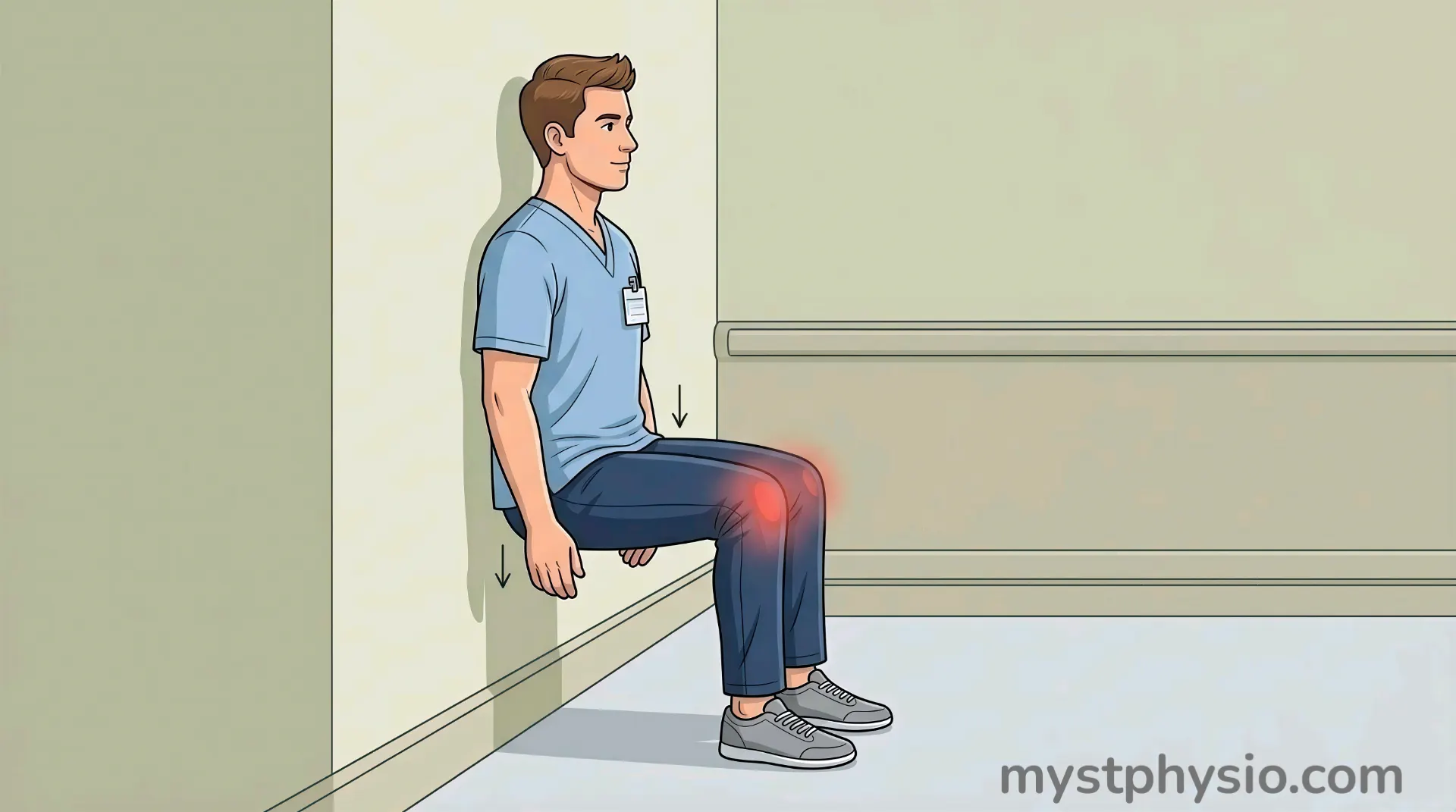
Isometric (eye-so-MET-rik) exercise means contracting the muscle without moving the joint. No movement. Just sustained tension.
For example: pressing your foot hard into a wall and holding for 45 seconds. The muscle works, the tendon is loaded, but nothing moves.
Why does this matter? Multiple studies suggest isometric contractions can reduce tendon pain within minutes. The exact mechanism isn’t fully understood yet, but the clinical effect is real and can be a useful tool when pain is high, allowing you to keep the tendon active without aggravating it.
Addressing Load Management – The Real Root Cause
Almost every case of tendinopathy comes back to one thing: the tendon was given more load than it was prepared for.
This happens when:
- You suddenly increase training volume (“too much too soon”)
- You return to activity after a break without building back gradually
- Your technique places unusual stress on a tendon
- You’re not recovering between sessions
Working with a sports medicine doctor or physiotherapist to understand your specific load patterns is, arguably, more important than any single exercise.
What About Shockwave Therapy?
Extracorporeal shockwave therapy (ESWT), a machine that delivers sound wave pulses into the tendon, has genuine evidence behind it for certain types of tendinopathy, particularly mid-portion Achilles tendinopathy and calcific (calcium-deposit) shoulder tendinopathy.
It’s not a magic fix. It works best as an adjunct, meaning alongside a good loading programme, not instead of one.
What About Injections?
Corticosteroid injections (a type of steroid injection directly into or around the tendon) used to be the go-to treatment. Evidence now suggests they can provide short-term pain relief but may actually worsen long-term outcomes and increase the risk of tendon rupture with repeated use.
A PRP injection (Platelet-Rich Plasma, where a small amount of your own blood is spun to concentrate growth factors, then injected back) has attracted a lot of attention. The evidence is mixed. Some trials show benefit; others show no difference from a placebo injection. The NHS does not routinely fund PRP for tendinopathy, and most guidelines treat it as an emerging rather than established treatment.
If someone suggests an injection, ask: “What does the current evidence say for my specific tendon?” The answer differs depending on location and stage of injury.
Things That Genuinely Don’t Help (Much)
- Prolonged rest alone – tendons need load. Resting without a return-to-load plan just delays recovery.
- Anti-inflammatory drugs (NSAIDs) like ibuprofen – tendinopathy in its chronic (long-term) stage is not primarily inflammatory, so anti-inflammatories have limited benefit beyond short-term comfort.
- Stretching the painful tendon aggressively – this can compress the tendon at its attachment point and worsen insertional (at-the-bone) tendinopathies in particular.
- Waiting it out without treatment – some cases do improve, but without addressing the load issue, many don’t.
When Should You See a Doctor?
Most people wait too long. If you’ve had tendon pain for more than 6 weeks, see a healthcare professional. Earlier if:
- Pain is severe or woke you from sleep
- There was a sudden “pop” or sharp pain – this could indicate a partial or full tendon tear
- The area is very swollen, red, or warm to touch
- Pain is affecting your ability to walk, work, or perform daily tasks
A doctor may arrange an ultrasound or MRI scan (types of medical imaging that show the inside of the body) to see the extent of tendon damage and rule out a tear.
RELATED: Cubital Tunnel Syndrome Physiotherapy Management Without Surgery
Living Well With Tendinopathy
A diagnosis of tendinopathy is not a life sentence. Many people, including professional athletes, recover fully. But recovery requires patience and the right approach.
A few things that genuinely help day-to-day:
- Track your pain levels on a 0-10 scale after activity. A slight increase (3-4 out of 10) during or after exercise is generally acceptable. Sharp spikes above 5, or pain that takes more than 24 hours to settle, suggest you’ve done too much.
- Keep moving – gentle, pain-monitored activity is almost always better than nothing.
- Sleep matters – tissue repair accelerates during sleep. Poor sleep genuinely impairs healing.
- Nutrition – adequate protein intake supports tendon repair. Some evidence supports supplementing with collagen (a protein that makes up much of the tendon’s structure) combined with Vitamin C before exercise, though research is still evolving.
Frequently Asked Questions (FAQs)
It depends on severity and location, but most people need 3-6 months of structured treatment for meaningful improvement. Severe or long-standing cases can take longer. Consistency with a loading programme matters more than speed.
In most cases, some discomfort during a properly guided exercise programme is expected and acceptable. The key is monitoring pain levels and keeping them within a manageable range. Exercising without guidance through sharp or severe pain is not recommended.
It can, especially if the underlying load management issue isn’t addressed. People who understand their triggers and manage their training load tend to have far fewer recurrences.
Mild cases sometimes settle with activity modification and self-managed exercises. But for persistent tendinopathy (more than 6-8 weeks), professional guidance significantly improves outcomes. It’s not just about doing exercises, it’s about doing the right exercises, at the right load, progressed at the right rate.
No. Tendinopathy refers to degeneration and damage within the tendon’s structure, but the tendon is still intact. A tear means the tendon fibres have partially or fully ruptured. Tears typically cause sudden, sharp pain and may require surgical review.
Yes. Higher body weight increases the compressive and tensile load on tendons, particularly in the lower limb (Achilles, patellar, gluteal). Even modest weight reduction can meaningfully reduce tendon load.
The Bottom Line
Tendinopathy is stubborn because tendons heal slowly, because pain disappears before repair is complete, and because rest alone doesn’t fix the underlying structural problem.
What works is progressive loading, building the tendon’s capacity gradually, under professional supervision, with patience. That’s not the quick fix most people want. But it’s the one that actually lasts.
Talk to your doctor or a physiotherapist to get a personalised assessment and loading programme for your specific tendon. Don’t guess. Don’t push through blindly. Get the right plan, then trust the process.
References
- Cook JL, Purdam CR. Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. British Journal of Sports Medicine. 2009;43(6):409-416.
- Beyer R, Kongsgaard M, Hougs Kjær B, et al. Heavy slow resistance versus eccentric training as treatment for Achilles tendinopathy. The American Journal of Sports Medicine. 2015;43(7):1704-1711.
- Rio E, Kidgell D, Purdam C, et al. Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. British Journal of Sports Medicine. 2015;49(19):1277-1283.
- Mani-Babu S, Morrissey D, Waugh C, Screen H, Barton C. The effectiveness of extracorporeal shock wave therapy in lower limb tendinopathy: a systematic review. The American Journal of Sports Medicine. 2015;43(3):752-761.
- Coombes BK, Bisset L, Vicenzino B. Efficacy and safety of corticosteroid injections and other injections for management of tendinopathy. The Lancet. 2010;376(9754):1751-1767.
- National Institute for Health and Care Excellence (NICE). Platelet-rich plasma injections for tendinopathy. Interventional procedures guidance [IPG715]. London: NICE; 2021.
- Andres BM, Murrell GA. Treatment of tendinopathy: what works, what does not, and what is on the horizon. Clinical Orthopaedics and Related Research. 2008;466(7):1539-1554.
- Dattilo M, Antunes HK, Medeiros A, et al. Sleep and muscle recovery: endocrinological and molecular basis for a new and promising hypothesis. Medical Hypotheses. 2011;77(2):220-222.
- Shaw G, Lee-Barthel A, Ross ML, Wang B, Baar K. Vitamin C-enriched gelatin supplementation before intermittent activity augments collagen synthesis. The American Journal of Clinical Nutrition. 2017;105(1):136-143.
This article is written for general informational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for guidance specific to your condition.